Keeping Clinicians Safe in High-Risk Care Areas
CAREFLOWTM STAFF DURESS CASE STUDY
As the only hospital in a busy urban area in New Jersey, leaders at this medical center understand the risk of violence against caregivers. They selected the Midmark CareFlow Real-Time Locating System (RTLS) Staff Duress solution to better protect staff and create a safer work environment.
PROACTIVE PROTECTION: ELEVATING SAFETY IN HIGH-RISK UNITS
Workplace violence is a serious occupational risk within healthcare. One in four nurses are assaulted,1 and caregivers who work with combative patients in behavioral health units, emergency departments or isolated areas of the hospital are particularly vulnerable. Tensions are high and circumstances are higher in these parts of the care continuum, placing caregivers in precarious situations that end too often in violence.
A newly hired security director at this New Jersey medical center placed top priority on the safety of staff in these higher risk areas. When the hospital received a Homeland Security grant, he petitioned to use the funding for a solution that could create a safer work environment for caregivers.
REAL DATA, REAL IMPROVEMENTS
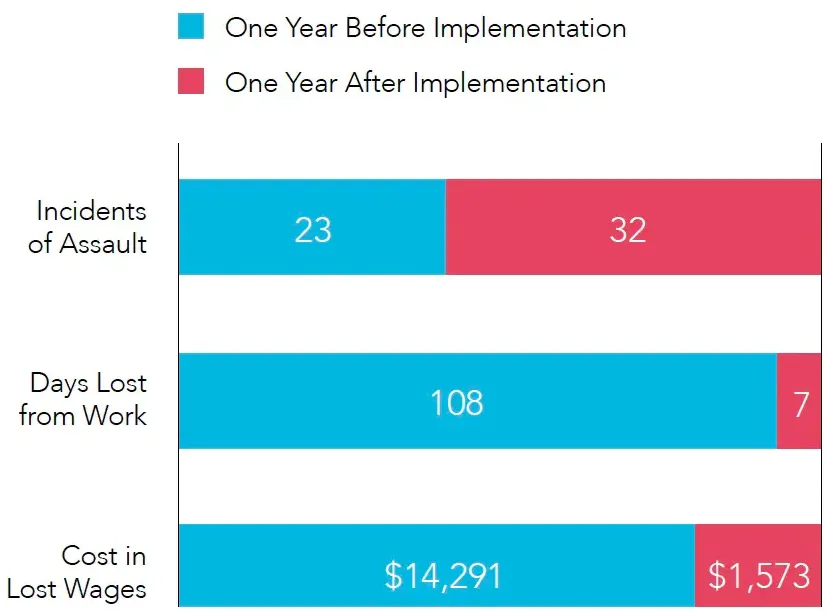
Despite a 39% increase in assaults on staff, post-implementation results revealed:
- 93.5% decrease in number of days lost from work
- 89% decrease in associated cost of wages
Many of our staff work in areas where they are sometimes alone with volatile patients. Previously, if a nurse needed help, she wouldn’t be able to get it right way. By pushing the badge button, not only does it alert other people, but the alert message also shows the nurse’s location.
-Director of Security
They selected CareFlow™ Staff Duress, a solution driven by RTLS technology and installed by the local Midmark RTLS Certified System Integrator.
The solution provides caregivers with badges that transmit real-time location information. When nurses, physicians and other hospital staff feel threatened, they simply press the badge button. Automatically, a message is sent to security detailing who they are and where they are, so help can be sent immediately to their location.
The Emergency Department was the first unit to implement CareFlow Staff Duress. It was quickly followed by the locked inpatient psychiatric unit and the outpatient psychiatric unit.
Staff location information is monitored at a central area within each unit, in addition to a house-wide security command center. Risk assessments, coupled with incident reporting from employee records, are used to monitor levels of workplace violence throughout the campus.
Spikes in reported incidents in other departments led the team to target additional areas for CareFlow expansion, which were funded by the hospital foundation in two separate grants.
With the expansions, more than 350 staff members received Midmark RTLS badges. When the badge button is pressed, it immediately signals an alert, triggering response protocols based on the treatment area from which it was initiated. Improving response times often lessens the severity of physical assaults.
The nurses in the medical center’s Emergency Department appreciate the security CareFlow provides. One mentioned, “Before, I had nothing to alert my coworkers if I was in trouble, but now I have this badge. It improves morale in the ED, knowing that help is just a button-push away.”
At the suggestion of The Joint Commission, the hospital conducted a review of assault data, comparing data from the year before they implemented CareFlow to the year after. Although assaults increased by 39% during the 12-month period after CareFlow was installed, the number of days lost from work decreased by 101 days.
The associated decrease in the cost of wages equated to $12,718, an 89% decrease. These results were published in The Joint Commission’s Leading Practice Library, in a report titled “Workforce Violence in Healthcare Not Always Preventable: A Plan for Mitigation.”2
“Many staff members report that they feel safer and more confident that they can press the button on the RTLS badge and get immediate help,” says one nurse. “Although we can’t prevent workplace violence, a system like [CareFlow] can lessen the aftermath of these incidents.”
2 “Workforce Violence in Healthcare Not Always Preventable,” The Joint Commission Leading Practice Library, 2016.