At the Core of Accuracy: Rethinking Temperature Measurement in Clinical Practice

By:
Clinical Education Manager, Midmark Corporation
October 22, 2025
Accurate, fast and non-invasive—three words every clinician wants to hear when it comes to vital signs acquisition. Temperature is often the first indicator of physiological change, yet how we measure it can vary significantly. As clinicians, we know that temperature measurement is not one-size-fits-all. The site and method we choose can influence the reliability of the result and, in turn, impact clinical decision making.
There are several non-invasive methods used to obtain temperature readings, including oral, axillary, tympanic and temporal artery. However, it’s important to remember that not all these methods measure core temperature, and depending on the site, the measurement of body temperature can vary by as much as 1°C.1 In fast-paced or high-acuity environments, that difference can affect how and when we respond to a patient’s condition. This variance is important in critical settings where early detection of fever or hypothermia may influence isolation protocols, diagnostic pathways or interventions.
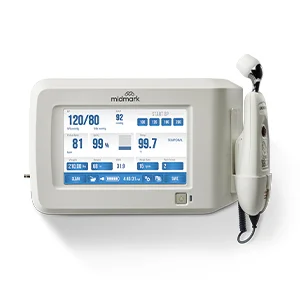
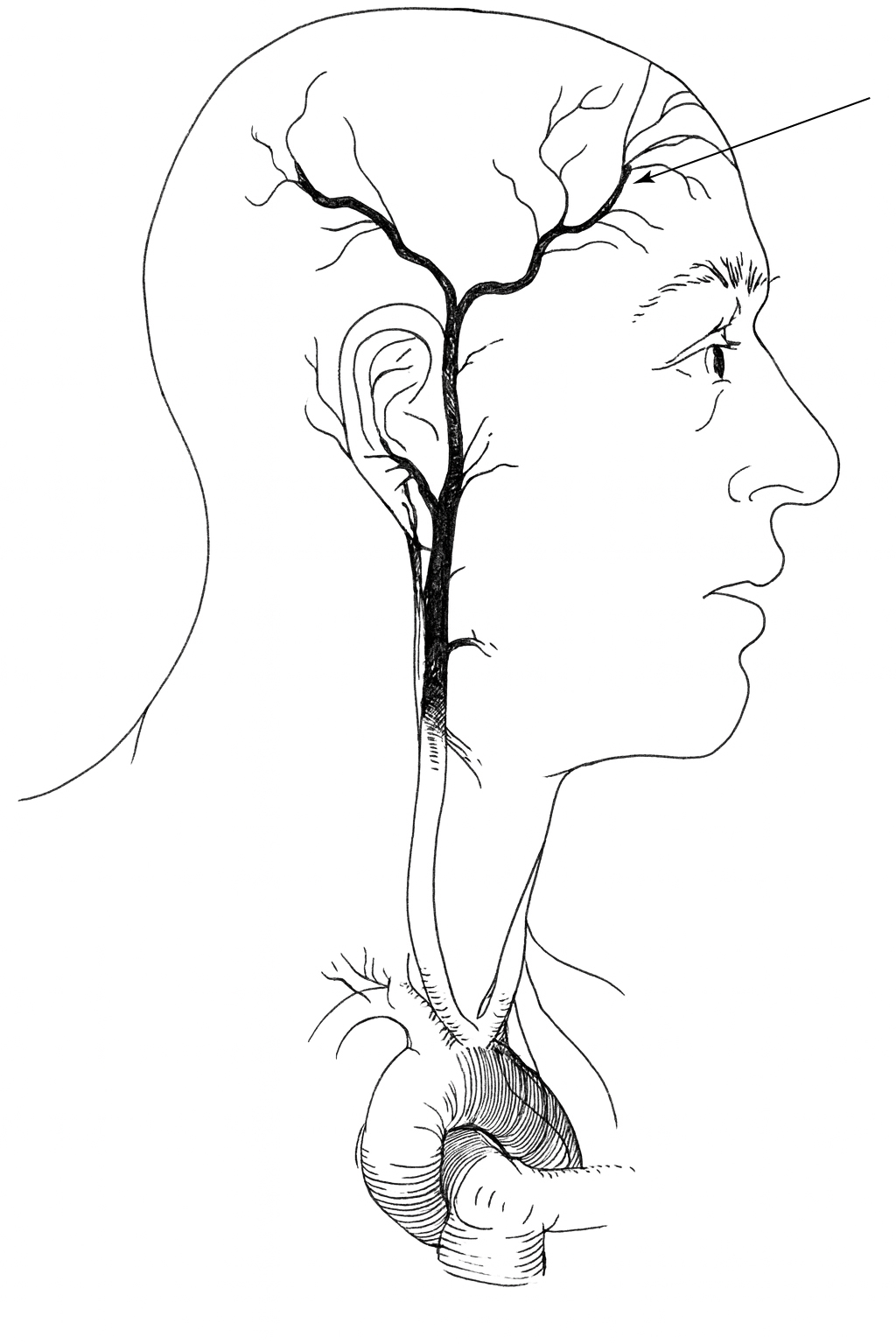
This blog explores how the Exergen® TemporalScanner® functions as a clinically relevant tool for obtaining accurate core temperature in a variety of patient care settings. Through a clinical lens, we’ll examine how temporal artery thermometry compares to other noninvasive methods, why core temperature matters in everyday decision-making, and how small differences in technique or modality can influence the bigger clinical picture.