Why Automated Vital Signs Acquisition Matters in Ambulatory Care

By:
Marketing Manager, Midmark Medical
May 4, 2026
Vital signs are some of the first data points captured during a patient visit and they directly inform clinical decision-making, risk stratification and longitudinal care. In many ambulatory settings, however, the workflow behind that data still relies on manual steps. Across a busy clinic, those steps can add up to slower room turnover, more documentation burden and less consistency from one encounter to the next.
Manual readings, disconnected devices and hand-entered documentation may feel familiar, but familiar does not always mean efficient. When vital signs collection depends on multiple handoffs and separate documentation steps, it can introduce variation, delay charting and create friction for both staff and patients.
For ambulatory care leaders, the question is not simply whether readings are captured manually or digitally. The more important question is whether the workflow is standardized, repeatable and connected to the patient record in a way that supports operational efficiency, staff confidence and the patient experience while improving confidence in the accuracy of the results used for clinical decision-making.
Manual vital signs workflows can create hidden friction
In many ambulatory care environments, vital signs are still captured through a mix of manual readings, standalone devices and later entry into the electronic medical record. Each individual step may seem small, but over the course of a full clinic day, those small steps can become a meaningful source of inefficiency.
When caregivers move between devices, jot down readings or return later to enter values into the chart, the process becomes more dependent on memory, timing and personal habits. That can slow patient flow, interrupt room turnover and add administrative burden during already demanding visits. More importantly, it can create inconsistencies that affect the accuracy and reliability of the data caregivers use to make clinical decisions.
This matters because vital signs acquisition is not an isolated task. It is part of a broader point-of-care workflow that influences how smoothly the visit moves from intake to documentation to care delivery. When that workflow is fragmented, the consequences extend beyond efficiency, affecting the quality of the information captured and the confidence caregivers have in acting on it.
Ambulatory care leaders are often evaluating more than device performance. They are looking at how the overall process affects:
- Workflow consistency
- Staff efficiency
- Documentation accuracy
- Patient throughput
- Patient experience
- Clinical outcomes
That broader view is what makes automated vital signs acquisition an important workflow conversation.
Manual processes can introduce variability and documentation risk
Even in well-run practices with experienced caregivers, manual workflows can create more opportunities for inconsistency before data ever reaches the chart.
When data collection and documentation happen as separate steps, there is greater risk that information may be delayed, omitted or entered incorrectly. Studies have reported an average 17% error rate in manual transcription of vital signs data, including omissions, incorrect entries and discrepancies between observed and recorded values1, highlighting how disconnected processes can affect documentation integrity.
For example, blood pressure accuracy depends on proper patient positioning, appropriate cuff size on a bare arm, a rest period before measurement and averaging repeat readings. When workflows are not standardized, these steps may be applied inconsistently across caregivers and encounters, which can affect the reliability of the recorded value.
Manual workflows can also introduce variation in how readings are captured and recorded from one team member to another. In fast-moving clinical settings, even small differences in technique or documentation habits can make it difficult to maintain consistency across rooms, caregivers and patient encounters.
That inconsistency can lead to downstream challenges such as:
- Delayed chart completion
- More rework when values are unclear or missing
- Less confidence in the integrity of recorded data
- Greater reliance on individual habits instead of standardized workflow
The issue is not a lack of clinical skill. The issue is that manual vital signs acquisition often depends on too many separate steps to reliably support a consistent, connected workflow.
Automated vital signs acquisition delivers more value at the point of care
The value of automation goes beyond faster readings. Automated vital signs acquisition becomes more meaningful when it happens at the point of care and supports a connected exam room workflow.
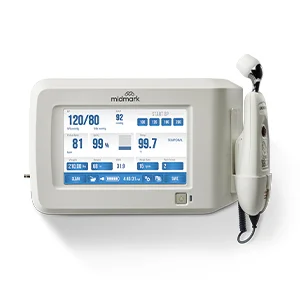
When blood pressure, temperature, SpO2, pulse rate and weight are captured at the point of care and transferred directly into the EMR, practices can reduce manual transcription steps and simplify documentation. Instead of treating vital signs collection and charting as separate activities, teams can support a more streamlined process from intake through clinical decision-making.
Midmark positions the digital vital signs device to automate capture of key measurements and support direct EMR integration. Studies show that bringing all vital signs capture, including weight, to the point of care with an automated device can save up to 69 seconds per patient in controlled workflow settings, depending on clinic design and implementation2.
In ambulatory care, gains like that can matter across every room, every caregiver and every patient visit. These improvements also support more reliable trend data over time, which is particularly important for conditions such as hypertension where diagnosis and treatment decisions depend on consistent, repeatable measurements rather than isolated readings.
A connected point-of-care workflow can help make vital signs acquisition:
- More standardized across rooms and users
- Less dependent on handwritten notes or delayed entry
- Better aligned with documentation needs
- More supportive of efficient patient flow
For ambulatory care leaders, that shifts the conversation. The opportunity is not just to replace a manual process with a digital one. It is to create a workflow that connects care delivery and data capture more effectively.
Connected workflows support consistency for staff and a smoother experience for patients
Automation should be evaluated not only by technical features, but by the operational outcomes it can support.
When workflows are standardized, staff can spend less time managing extra steps and more time focusing on the patient. Fewer manual tasks can help reduce cognitive load, improve confidence in documentation and create a more repeatable process across the care team. Patients benefit as well. When automated vital signs acquisition is integrated into the point-of-care workflow, the visit can feel more organized and less fragmented. Teams are not moving between disconnected steps or returning later to complete documentation. Instead, the process can flow more naturally within the exam room.
This is where the care environment becomes especially important. A connected exam room workflow can help support:
- More consistent clinical processes
- Better documentation flow
- Improved staff efficiency
- A more seamless patient experience
Rather than viewing vital signs acquisition as a standalone task, practices can view it as part of a broader strategy to improve how care is delivered at the point of care.
What to look for in an automated vital signs workflow
As practices consider moving from manual to automated vital signs acquisition, the decision should go beyond device specifications alone. The better question is whether the solution fits the care environment and supports broader operational goals.
Ambulatory care leaders should look for a workflow that can:
- Support direct EMR integration to reduce or replace manual entry
- Fit naturally into point-of-care processes
- Help standardize capture across caregivers, rooms and patient encounters
- Support a broader connected diagnostics strategy over time
The most effective solution is not simply one that digitizes readings. It is one that helps practices create a more connected, efficient and repeatable process around those readings.
A better workflow starts with a better connection between care and data
Moving from manual to automated vital signs acquisition is about more than convenience. It is about reducing friction, improving consistency and helping care teams work more efficiently at the point of care.
As ambulatory practices look for ways to strengthen operations without adding complexity, connected workflows offer a practical path forward. When vital signs capture is integrated more closely with the exam room and the EMR, practices can support a better experience for staff, more confidence in documentation and a smoother experience for patients.
Explore how connected diagnostic solutions can help simplify automated vital signs acquisition at the point of care. Download the digital vital signs brochure and visit the Midmark Medical resource library for more workflow insights.
See the Research:
- 3 Signs It’s Time to Upgrade Your Vital Signs Process
- Digital Vital Signs Device Brochure
- Midmark Medical Resource Library
- Digital Diagnostics Connected Solutions
Sources:
1 Fieler, V. K., Jaglowski, T., & Richards, K. (2013). Eliminating errors in vital signs documentation. Comput Inform Nurs, 31(9), 422-427; quiz 428-429.doi:10.1097/01. NCN.0000432125.61526.27 PMID:24080751
2 https://www.ncbi.nlm.nih.gov/pubmed/30715088